Professor Matthias Zilbauer
Intestinal stem cell biology
Clinical Professor of Paediatric Gastroenterology
Departmental affiliation:
- University Department of Paediatrics
- Department of Paediatric Gastroenterology, Hepatology and Nutrition (Cambridge University Hospitals)
Email: mz304@cam.ac.uk
Biography
Matthias Zilbauer completed his medical training and obtained his MD degree from the University of Mainz, Germany and obtained a PhD in mucosal immunology from the Institute of Child Health at University College London (UCL, UK) investigating innate immunity of the intestinal epithelium. Matthias completed his clinical training in paediatrics as well as paediatric gastroenterology following training in several leading international centres based in the UK and Germany. In 2013, Matthias was appointed University Lecturer and Honorary Consultant in Paediatric Gastroenterology the University of Cambridge and Cambridge University Hospitals. Supported by an MRC New Investigator Research Award, Matthias established his research group with a focus on the role of epigenetic mechanisms in regulating intestinal epithelial stem-cell function in health, development, and Inflammatory Bowel Diseases. In 2022 Matthias joined the Cambridge Stem Cell Institute as a group leader. In 2023 he was named Clinical Professor of Paediatric Gastroenterology.
Funding: Medical Research Council (MRC, UK), Helmsley Charitable Trust, Action Medical Research, Great Ormond Street Hospital Charity
Research
The Zilbauer group's main research interest lies in the field of human intestinal epithelial stem cell biology during development, health and related diseases such as Inflammatory Bowel Diseases (IBD) and Necrotising Enterocolitis (NEC). A particular focus lies on the role of role of epigenetic mechanisms (i.e. DNA methylation) in regulating gene expression and cellular function of the human intestinal epithelium and the implication of epigenetic (re)programming on development and disease pathogenesis.
As one of the main experimental models, they use human mucosa derived intestinal epithelial organoids. Over the past 8 years, they have generated a large living biobank containing >1000 frozen organoid lines that form the basis for future translational research efforts. In addition to organoids derived from intestinal mucosal samples, induced pluripotent stem cells (iPSCs) can be differentiated into intestinal epithelium.
Current projects focus on the development of clinical biomarkers to guide treatment of children diagnosed with Inflammatory Bowel Diseases, test novel treatments targeting the intestinal epithelium using our organoid model and further develop 2D and 3D culture systems which allow complex co-culture of the intestinal epithelium with other cell types (e.g. immune and stromal cells) as well as the intestinal microbiota.
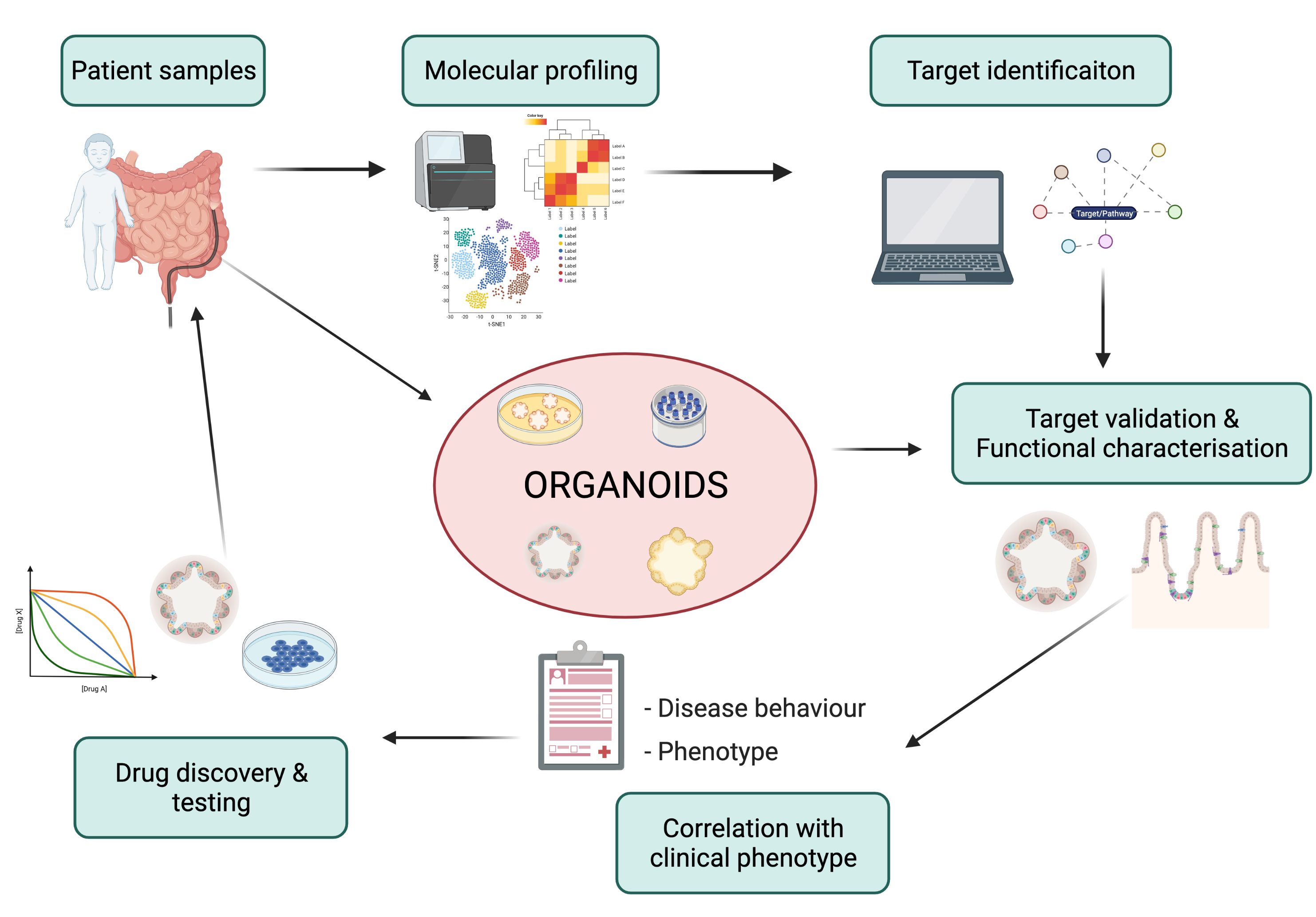
Figure 1: Use of human intestinal epithelial organoids as translational research tools for the development of novel treatment approaches.
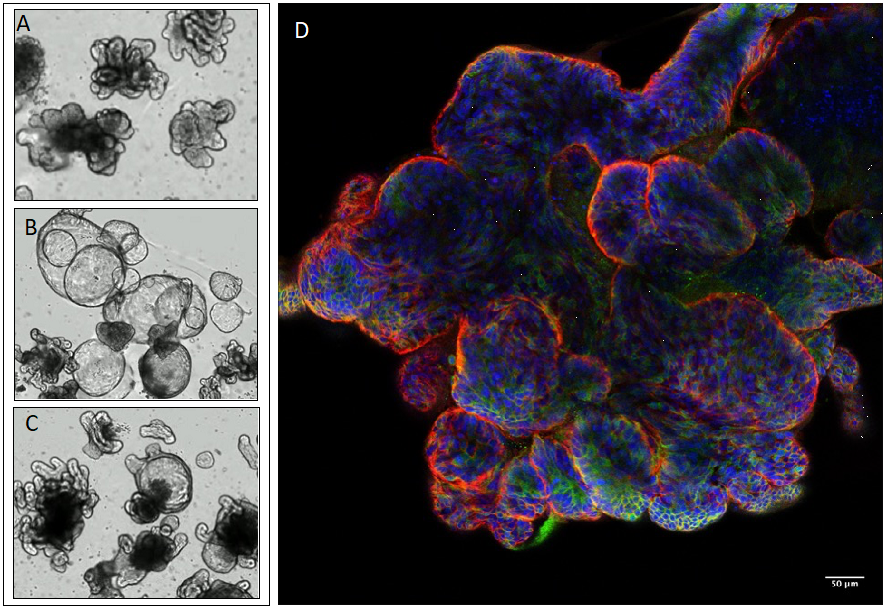
Figure 2: Brightfield images of Human Intestinal Epithelial Organoids (IEOs) derived from A) Terminal Ileum B) Duodenum C) Sigmoid Colon. D) Fluorescent image of organoid derived from Terminal Ileum and stained for Nuclei (blue), LGR5 (green) and E-cadherin (red)
Zilbauer Group photo
Plain English
The intestinal epithelium forms the most inner layer of the human intestine. In addition to playing an important role in helping to digest and absorb nutrients and water, the epithelium also provides a crucial barrier that protects us from potentially harmful bacteria or toxins contained in our daily diet. Impaired function of the epithelium can lead to disease for example chronic gut inflammation (Crohn’s Disease and Ulcerative Colitis). Such chronic inflammatory bowel diseases increasingly affect small children and have a devastating impact on their lives. Although we do not understand why more and more people are diagnosed with these conditions, it seems clear that changes in our environmental play a key role. That is why we are studying the potential role of ‘epigenetic mechanisms’ in gut diseases. These ‘epigenetic mechanisms’ can switch genes on or off and thereby allow our cells to adapt to changes in our environment. This is important to allow our body to function, but it can also lead to disease if something goes wrong.
If we understand the epigenetic changes in the gut epithelium of patients suffering from gut diseases we can find ways to ‘reset’ the epigenome or use medications to prevent the consequences causing damage to the gut.
Key publications
-
Edgar RD, Perrone F, Foster AR, Payne F, Lewis S, Nayak KM, Kraiczy J, Cenier A, Torrente F, Salvestrini C, Heuschkel R, Hensel KO, Harris R, Jones DL, Zerbino DR, Zilbauer M. Cell Mol Gastroenterol Hepatol. 2022;14(6):1295-1310. doi: 10.1016/j.jcmgh.2022.08.008. Epub 2022 Aug 28.
-
Cells of the human intestinal tract mapped across space and time.
Elmentaite R, Kumasaka N, Roberts K, Fleming A, Dann E, King HW, Kleshchevnikov V, Dabrowska M, Pritchard S, Bolt L, Vieira SF, Mamanova L, Huang N, Perrone F, Goh Kai'En I, Lisgo SN, Katan M, Leonard S, Oliver TRW, Hook CE, Nayak K, Campos LS, Domínguez Conde C, Stephenson E, Engelbert J, Botting RA, Polanski K, van Dongen S, Patel M, Morgan MD, Marioni JC, Bayraktar OA, Meyer KB, He X, Barker RA, Uhlig HH, Mahbubani KT, Saeb-Parsy K, Zilbauer M, Clatworthy MR, Haniffa M, James KR, Teichmann SA.Nature. 2021 Sep;597(7875):250-255. doi: 10.1038/s41586-021-03852-1. Epub 2021 Sep 8.
-
Elmentaite R, Ross ADB, Roberts K, James KR, Ortmann D, Gomes T, Nayak K, Tuck L, Pritchard S, Bayraktar OA, Heuschkel R, Vallier L, Teichmann SA, Zilbauer M.Dev Cell. 2020 Dec 21;55(6):771-783.e5. doi: 10.1016/j.devcel.2020.11.010. Epub 2020 Dec 7.
-
High-Resolution mRNA and Secretome Atlas of Human Enteroendocrine Cells.
Beumer J, Puschhof J, Bauzá-Martinez J, Martínez-Silgado A, Elmentaite R, James KR, Ross A, Hendriks D, Artegiani B, Busslinger GA, Ponsioen B, Andersson-Rolf A, Saftien A, Boot C, Kretzschmar K, Geurts MH, Bar-Ephraim YE, Pleguezuelos-Manzano C, Post Y, Begthel H, van der Linden F, Lopez-Iglesias C, van de Wetering WJ, van der Linden R, Peters PJ, Heck AJR, Goedhart J, Snippert H, Zilbauer M, Teichmann SA, Wu W, Clevers H.Cell. 2020 Aug 20;182(4):1062-1064. doi: 10.1016/j.cell.2020.08.005.
-
Gasparetto M, Payne F, Nayak K, Kraiczy J, Glemas C, Philip-McKenzie Y, Ross A, Edgar RD, Zerbino DR, Salvestrini C, Torrente F, Ventham NT, Kalla R, Satsangi J, Sarkies P, Heuschkel R, Zilbauer M. Gastroenterology. 2021 Jan;160(1):232-244.e7. doi: 10.1053/j.gastro.2020.08.017. Epub 2020 Aug 16.
-
The landscape of somatic mutation in normal colorectal epithelial cells.
Lee-Six H, Olafsson S, Ellis P, Osborne RJ, Sanders MA, Moore L, Georgakopoulos N, Torrente F, Noorani A, Goddard M, Robinson P, Coorens THH, O'Neill L, Alder C, Wang J, Fitzgerald RC, Zilbauer M, Coleman N, Saeb-Parsy K, Martincorena I, Campbell PJ, Stratton MR.Nature. 2019 Oct;574(7779):532-537. doi: 10.1038/s41586-019-1672-7. Epub 2019 Oct 23.PMID: 31645730
-
Kraiczy J, Ross ADB, Forbester JL, Dougan G, Vallier L, Zilbauer M. Cell Mol Gastroenterol Hepatol. 2019;7(2):285-288. doi: 10.1016/j.jcmgh.2018.10.008. Epub 2018 Oct 23.
-
Kraiczy J, Nayak KM, Howell KJ, Ross A, Forbester J, Salvestrini C, Mustata R, Perkins S, Andersson-Rolf A, Leenen E, Liebert A, Vallier L, Rosenstiel PC, Stegle O, Dougan G, Heuschkel R, Koo BK, Zilbauer M. Gut. 2019 Jan;68(1):49-61. doi: 10.1136/gutjnl-2017-314817. Epub 2017 Nov 15
-
Howell KJ, Kraiczy J, Nayak KM, Gasparetto M, Ross A, Lee C, Mak TN, Koo BK, Kumar N, Lawley T, Sinha A, Rosenstiel P, Heuschkel R, Stegle O, Zilbauer M. Gastroenterology. 2018 Feb;154(3):585-598. doi: 10.1053/j.gastro.2017.10.007. Epub 2017 Oct 12.